Diabetic Foot Issue
The Problem
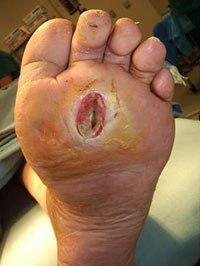 For people with diabetes, having too much glucose (sugar) in their blood for a long time can cause some serious complications, including foot problems.
For people with diabetes, having too much glucose (sugar) in their blood for a long time can cause some serious complications, including foot problems.
Foot problems are common in people with diabetes. You might be afraid you’ll lose a toe, foot, or leg to diabetes, or know someone who has, but you can lower your chances of having diabetes-related foot problems by taking care of your feet every day. Managing your blood glucose levels, also called blood sugar, can also help keep your feet healthy.
Several classification systems have been used. A good classification system takes into account the major risk factors involved in causing a diabetic foot problem–namely vasculopathy, neuropathy and immunopathy, elements of the diabetic foot triad. A good classification is useful as a guide to the treatment needed for each patient. One of the most common classification include:
Table 1: Wagner-Meggitt Wound Classification
| Grade | Description of ulcer |
| Grade 0 | Pre- or post-ulcerative lesion completely epithelialised |
| Grade 1 | Partial/full-thickness ulcer confined to the dermis, not extending to the subcutis |
| Grade 2 | Ulcer of the skin extending through the subcutis with exposed tendon or bone No abscess formation or osteomyelitis |
| Grade 3 | Deep ulcer with abscess formation or osteomyelitis |
| Grade 4 | Localised gangrene of the toes or partial foot gangrene |
| Grade 5 | Whole foot gangrene |
Figure 1: Wagner-Meggitt Wound Classification.
| Grade 0:
No open lesion |
Grade 1:
Superficial ulcer |
Grade 2:
Deep ulcer |
Grade 3:
Deep Abscess/OM |
Grade 4:
Partial foot gangrene |
Grade 5:
Whole foot gangrene |
Treatment
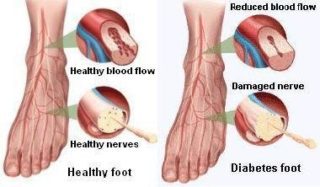 Dr. foot offers a full range of services for treating lower-extremity complications of diabetes, regular consultation, treatment and education to prevent foot problems and amputation whenever possible with special emphasis on foot problems. We use the latest research and treatment option to keep our patients on their feet.
Dr. foot offers a full range of services for treating lower-extremity complications of diabetes, regular consultation, treatment and education to prevent foot problems and amputation whenever possible with special emphasis on foot problems. We use the latest research and treatment option to keep our patients on their feet.
Successful treatment of diabetic foot ulcers consists of addressing these three basic issues:
- infection control
- Patients with mild infections can be treated in outpatient settings with oral antibiotics that cover skin flora including streptococci and Staphylococcus aureus.
- For moderate-to-severe infections, patients should be hospitalized for parenteral antibiotic therapy.
- Duration of therapy should be individualized. For those treated in outpatient settings with oral antibiotics, duration of treatment is usually 7-14 days. In those treated parenterally but without osteomyelitis, 2-4 weeks is sufficient. Longer duration of therapy is required for those with osteomyelitis—4-6 weeks at a minimum is suggested. Duration of treatment may be shortened in those patients who undergo amputation as part of the treatment regimen.
- Offloading
- Foot ulcers are caused by an imbalance between excessive pressure on the sole of the foot and repetitive stress from walking. Common methods to offload pressure on the foot include: bed rest, the use of a wheel chair, crutches, total contact casts, felted foam, half shoes, therapeutic shoes, custom splints, and removable cast walkers.
- Debridement
- Any dead tissue should be removed from the wound, as required, using a sharp tissue nipper or scalpel or a curette. Finger pressure may be applied to the wound to help control bleeding. The wound may then be probed to check for underlying tissue and infection. Following adequate debridement, the wound can be dressed and pressure offloaded as required. At follow-up, the absence of undermining of the wound edges is a good sign that the wound has been appropriately offloaded.
- Conservative Treatment
- Neuropathy treatment: Good control of diabetes over time is the key to treating diabetic neuropathy. There is no cure for neuropathy, but keeping your blood sugar within a target range can reduce symptoms and prevent them from getting worse.
- Medicinessuch as pain relievers or creams to relieve pain. Prescription medicines often used to reduce pain from diabetic neuropathy may include medicines that are more commonly used to treat depression, such as tricyclic antidepressants and the antidepressant duloxetine hydrochloride, and medicines that control seizures, such as pregabalin and gabapentin. These medicines may be tried to reduce your pain even though you do not have depression or seizures.
- Complementary therapiessuch as acupuncture and biofeedback.
- Physical therapysuch as exercises, stretching, and massage. If you are told to use heat or ice, be careful. Neuropathy can make it hard for you to feel changes in temperature.
- Transcutaneous electrical nerve stimulation (TENS),which is a type of therapy that reduces pain by applying brief pulses of electricity to nerve endings in the skin
- Hyperbaric Oxygen There is strong evidence that fibroblasts, endothelial cells, and keratinocytes are replicated at higher rates in an oxygen-rich environment. Moreover, leukocytes kill bacteria more effectively when supplied by oxygen. It is also known that fibroblasts from diabetic individuals show diminished cell turnover in comparison with those from nondiabetic persons. Based on these data, the idea was that the administration of oxygen at high concentrations might accelerate wound healing in diabetes. Treatment with hyperbaric oxygen therapy involves the intermittent administration of 100% oxygen at a pressure greater than that at sea level. It is performed in a chamber with the patient breathing 100% oxygen intermittently while the atmospheric pressure is increased to 2–3 atmospheres for a duration of 1–2 h. A full course involves 30–40 sessions. A small amount of data suggests significant reduction of the ulcer area as well as reduction of the risk for major amputation. Hyperbaric oxygen can be applied as an adjunctive therapy for patients with severe soft-tissue foot infections and osteomyelitis who have not responded to conventional treatment. Adverse effects include barotrauma to the ears and sinuses, pneumothorax, transient changes in visual acuity, and seizures. Furthermore, a recent systematic review by the National Institute for Health and Clinical Excellence (NICE) Guidelines Development Group in the UK concluded that the available data are insufficient to demonstrate that hyperbaric oxygen therapy is cost-effective.
- Surgery
The removal of devitalized tissue to control infection and creation of an environment favorable for healing, while maximizing the structural and physical integrity of the foot, is the central goal of surgical intervention in treating diabetic foot infections.
Surgery may be recommended if the foot deformity puts the patient at a high risk for ulcers, or if protective shoe wear is not effective. Unstable fractures and dislocations also require surgery to heal.


